Melanoma
Overview
Melanoma Overview
Melanoma, or malignant melanoma, is a serious skin cancer that occurs when the DNA in certain skin cells becomes damaged. Melanoma is a cancer of the melanocytes, the cells in your skin that produce melanin (pigment). However, melanomas can also develop in any organ or body part that has melanocytes, such as your eyes, nose, throat and other areas of your body. Genetic predispositions and exposure to UV radiation from the sun or tanning beds dramatically increase your risk of developing melanoma.
Although historically diagnosed primarily in people ages 40 and over, melanoma seems to be increasing, especially in females under 40. While it’s diagnosed in fewer than 200,000 people each year in the United States, it remains potentially life-threatening if not caught early and treated before the cancer spreads (metastasizes) to other parts of the body.
Anyone can develop melanoma, but those at the highest risk have fair skin, fair hair and light-colored eyes because they have less pigment in their skin to protect them from harmful UV rays. Those who freckle and burn easily are also at a higher risk for the same reason. Those who live at higher elevations or closer to the equator are also at a higher risk because they have more UV radiation exposure. Additional risk factors include those who have:
- A family history of melanoma
- A weakened immune system
- Had excessive UV light exposure
- A history of one or more sunburns
- More than 50 ordinary looking moles
- Unusual looking moles with irregular borders or a mix of colors (dysplastic nevi)
Although less common, “hidden” melanoma (melanoma in areas that do not receive much UV exposure, like the buttocks or the soles of your feet) sometimes occurs. Hidden melanomas are more common in people with darker skin.
Symptoms
Melanoma Symptoms
Visible Melanomas
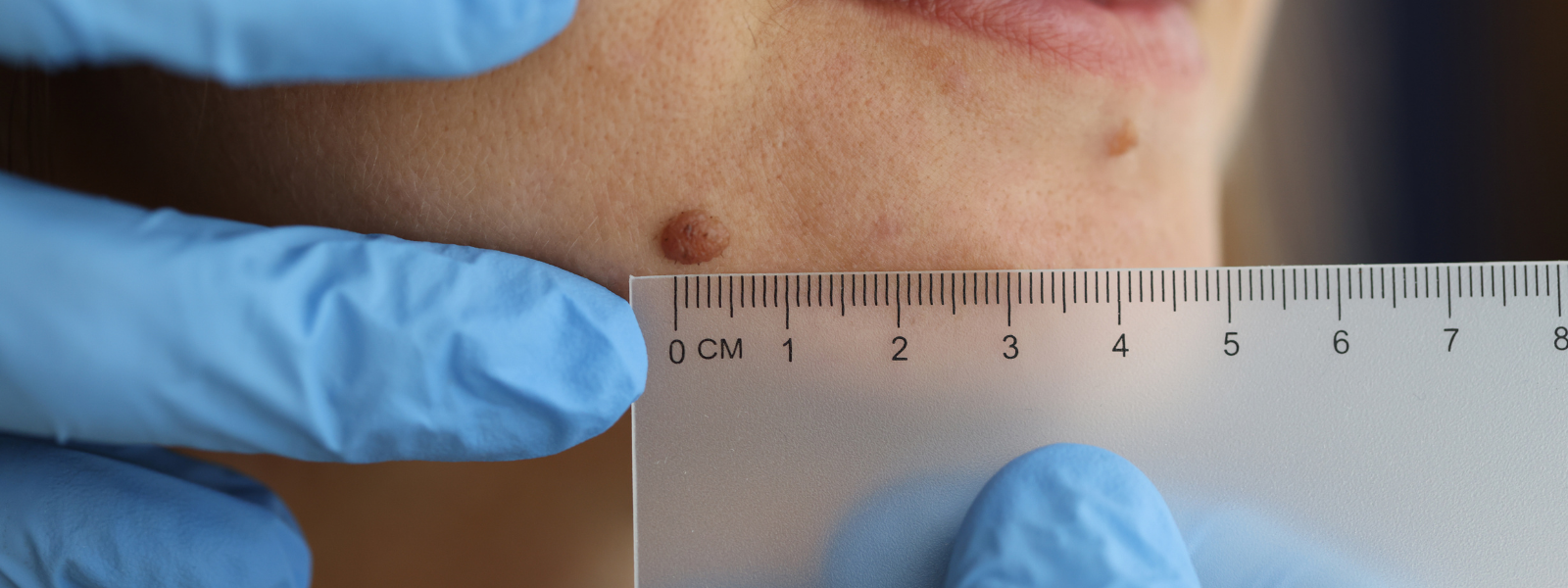
Most normal moles are uniform in color (tan or brown), round or oval with a smooth and distinct border, and smaller than 6 mm. Frequently, changes in existing moles, skin pigmentation or an unusual-looking growth are the first signs of melanoma. Other signs to look for include the ABCDEs of melanoma:
Asymmetry
The mole looks different from one side to the other side
Border Irregularity
The mole is uneven or has jagged edges
Color
The mole has different colors and patterns
Diameter
The mole may be larger than a typical mole, almost 6 mm in size (size of a pencil eraser) or larger
Evolving
The mole changes colors, size and texture, and it might also bleed
Hidden melanomas
Hidden melanomas are not easy to see, so you might need help looking in places you can’t easily see. There are three main types of hidden melanomas:
Acral-lentiginous melanoma
A rare form of hidden melanoma most common in black and dark-skinned people and people of Asian descent. Sometimes you may find these hidden melanomas:
- Between the toes
- On the soles of the feet
- On the palms of the hands
- Under a fingernail or toenail
Mucosal melanoma
Develops in the mucous membrane and can appear in the:
- Nose
- Mouth
- Throat (esophagus)
- Digestive tract
- Urinary tract
- Vagina
- Anus
Ocular (eye) melanoma
Usually occurs in the uvea, the layer beneath the white of the eye. Vision change is typically the first sign of ocular melanoma.
Diagnosis
Melanoma Diagnosis
Diagnosis begins with an examination where your doctor will ask you questions about your and your family’s medical history and examine your skin for any signs of melanoma. If your doctor suspects melanoma, they will want to biopsy the suspicious area to verify it is cancer. Your doctor will choose from three kinds of biopsies depending on your situation. In most cases, the doctor will want to remove the entire growth by doing one of the following procedures:
- An excisional biopsy uses a scalpel to remove the entire suspicious mole with a small margin of healthy tissue around it.
- A punch biopsy uses a circular blade pressed into the skin around the suspicious mole to remove it.
- A shave biopsy uses a broad razor blade to remove the suspicious mole with a small margin of healthy tissue around it.
Your doctor will send the sample to a lab for examination. If you are diagnosed with melanoma, the next step is to determine the cancer stage, which helps you and your doctor design your treatment plan.
The pathologist determines the stage based on the thickness, if lymph nodes are involved, or if cancer appears to have spread (metastasized) to other parts of the body besides the skin. If the melanoma is thick or has spread, your doctor may recommend additional tests. These tests include:
- A sentinel node biopsy if it has spread to lymph nodes. The doctor injects dye into the area where they removed the cancer. The dye flows to nearby lymph nodes, and the first nodes to absorb the dye are removed and tested to see if cancer has spread.
- If the melanoma is advanced, the doctor may order imaging tests such as x-rays, CT scans or PET scans to help strategize your treatment plan.
Treatments
Melanoma Treatments
Treatment for melanoma depends on its size, stage, location and the patient’s overall health.
Chemotherapy
Chemotherapy is delivered orally, intravenously or both and uses a mix of chemicals to target any quickly dividing cells.
Immunotherapy
Immunotherapy drugs can help you fight cancer. Sometimes, cancer cells produce proteins that help them hide from your immune system. Immunotherapy drugs block cancer’s ability to hide, allowing your body to see the cancerous cells.
Radiation therapy
Radiation therapy uses high-energy beams to treat the lymph nodes or other body parts where surgery isn’t feasible.
Surgery
Surgery can remove (excise) cancer from the affected area and part of the healthy tissue. The surgeon may also remove nearby lymph nodes depending on how advanced the cancer is.
Targeted therapy
Targeted therapy works differently than chemotherapy by specifically targeting weaknesses in melanoma cells.
Specialists

