Psoriasis
Overview
Psoriasis Overview
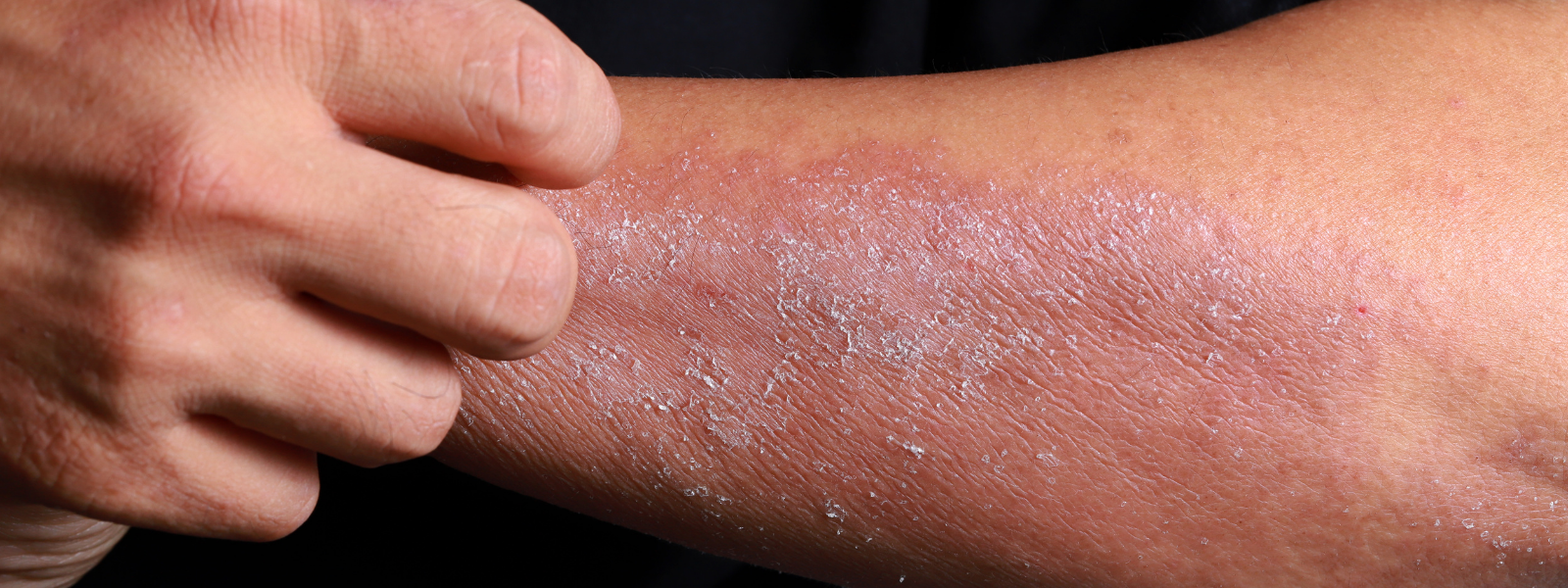
Psoriasis is a common skin condition with more than 3 million cases diagnosed each year in the United States. Psoriasis causes itchy red patches that you will most commonly find on your elbows, knees, torso and scalp.
Psoriasis is a long-term (chronic) disease, cycling with flare-ups lasting for a few weeks or months, then going away for a while before flaring up again. There is no cure for psoriasis, but treatments, lifestyle changes and coping strategies can help you effectively manage your psoriasis symptoms.
Types
Psoriasis is an autoimmune disorder that causes your skin to regenerate faster than usual. The most common type of psoriasis is plaque psoriasis, resulting in scales and itchy red patches on your skin.
The seven types of psoriasis are:
Erythrodermic
Nail psoriasis
Guttate psoriasis
Plaque psoriasis
Inverse psoriasis
Pustular psoriasis
Causes and Triggers
Researchers believe genetics and environmental factors play a role in developing psoriasis, which is not contagious. If environmental factors are the primary cause of your psoriasis, then you may go years without experiencing symptoms.
Some possible environmental triggers for flare-ups include:
- Strep throat or other infections
- Scrapes, cuts, bug bites or sunburn
- Excessive alcohol consumption
- Smoking and exposure to secondhand smoke
- Emotional situations that cause stress or depression
- Rapid withdrawal from oral or systemic corticosteroids
- Some medications, such as lithium, antimalarial drugs or those for high blood pressure
Risks
Having psoriasis may put you at a greater risk of developing:
- Psoriatic arthritis, which causes pain, stiffness and swelling in and around the joints
- Eye conditions like conjunctivitis, blepharitis and uveitis
- Inflammatory bowel disease (Crohn’s disease)
- Cardiovascular disease
- High blood pressure
- Type 2 diabetes
- Obesity
- Celiac disease
- Low self-esteem
- Depression
Although anyone can develop psoriasis, you may be at a greater risk of developing it if you have a family history of psoriasis. Psoriasis can begin at any age, but those ages 20 – 30 and 50 – 60 are most likely to see initial flare-ups at these ages.
Symptoms
Psoriasis Symptoms
Psoriasis symptoms vary by type.
Erythrodermic psoriasis
The least common type of psoriasis, erythrodermic psoriasis can cover the entire body with a red, peeling rash that may cause intense burning and itching.
Guttate psoriasis
Primarily seen in children and young adults, guttate psoriasis is usually triggered by a bacterial infection such as salmonella, strep throat or pneumonia. Look for small, drop-shaped, scaly lesions on your arms, legs or torso.
Inverse psoriasis
Inverse psoriasis causes smooth patches of red skin in the skin folds of your groin, buttocks and breasts. These patches may worsen with friction and sweating.
Nail psoriasis
Nail psoriasis can cause nail pitting, abnormal nail growth and discoloration. Your nails may separate from the nail bed (onycholysis), and in severe cases, your nail beds may crumble.
Plaque psoriasis
The most common type of psoriasis, plaque psoriasis can cause tender or itchy dry, raised, red skin patches (lesions) that may also have silvery scales. These lesions usually appear on elbows, knees, lower back and scalp.
Psoriatic arthritis
Psoriatic arthritis causes swollen, painful joints, stiffness, and progressive joint damage. Joint symptoms may be the first or only sign of psoriasis, though sometimes, changes in your nails are the only visible symptoms.
If left untreated, psoriatic arthritis can lead to permanent joint damage.
Pustular psoriasis
This rare form of psoriasis causes pus-filled lesions in extensive patches known as generalized pustular psoriasis. Pustular psoriasis can also occur in smaller areas like the palms of the hands and the soles of the feet.
Diagnosis
Psoriasis Diagnosis
Your doctor will ask questions about your symptoms and your and your family’s medical history. They will look at your skin, nails and scalp and may take a small skin sample (biopsy) to examine under a microscope.
Treatments
Psoriasis Treatments
Treatment for psoriasis helps remove scales and keep excessive skin cells from growing.
Which treatments you use depend on how severe the psoriasis is and how responsive it has been to previous therapy. You might need to try different drugs or a combination of treatments before finding an approach that works for you. Usually, however, the disease returns to some degree as it is chronic.
Light therapy (Phototherapy)
Phototherapy to expose your skin to specific amounts of artificial light is often among the first choices in treating moderate to severe psoriasis and can be used alone or combined with other treatments.
Light therapy options include:
UVB broadband
Using controlled doses of UVB broadband light from an artificial light source is an effective way to treat single patches, widespread psoriasis and psoriasis that does not improve with topical treatments.
UVB narrowband
UVB narrowband therapy has replaced broadband therapy in many places as it may be more effective.
Psoralen plus ultraviolet A (PUVA)
This treatment works by taking a light-sensitizing medication before exposing your skin to UVA light. UVA light can penetrate deeper into your skin than UVB light, and psoralen makes the skin more receptive to UVA exposure.
Excimer laser
This treatment uses an intense UVB light to target only the affected skin, making it a good option for smaller areas.
Topical therapy
Corticosteroids
Creams, lotions, ointments, gels, sprays, foams or shampoos containing corticosteroids treat mild to moderate psoriasis. Long-term use or overuse of potent corticosteroids can cause skin to thin, and topical corticosteroids may stop working over time.
Vitamin D analogues
Work by slowing the growth of skin cells.
Retinoids
Available as a gel or cream that you apply once or twice a day. Be sure to let your doctor know if you are pregnant, trying to get pregnant or breastfeeding.
Calcineurin inhibitors
These work by reducing inflammation and plaque buildup and are good for use on thin skin where retinoids and steroid creams may cause harmful effects or irritation.
Salicylic acid
Shampoos can reduce the itching and scaling of scalp psoriasis.
Coal tar
Reduces itching, scaling and inflammation and is available in shampoos, creams and oils.
Medications
If other treatments have not worked, oral or injected (systemic) medications may work better for you.
Some possible medicines your doctor may prescribe include the following. Be sure to ask your doctor about the risks and benefits of each treatment option.
Retinoid pills*
Help reduce the production of excess skin cells.
Methotrexate*
Reduces inflammation and decreases the production of skin cells. Men and women should stop taking methotrexate at least three months before attempting to conceive.
Cyclosporine*
Taken orally for severe psoriasis and works by suppressing your immune system.
Biologics
Alter your immune system, disrupting the cycle.
Let your doctor know if you are pregnant, trying to become pregnant or breastfeeding.
Lifestyle changes
Studies show that decreasing alcohol intake and cessation of smoking may help reduce the severity of psoriasis.
Additionally, weight loss in overweight or obese individuals may also decrease the severity of psoriasis.
Specialists

