Eczema (Atopic Dermatitis)
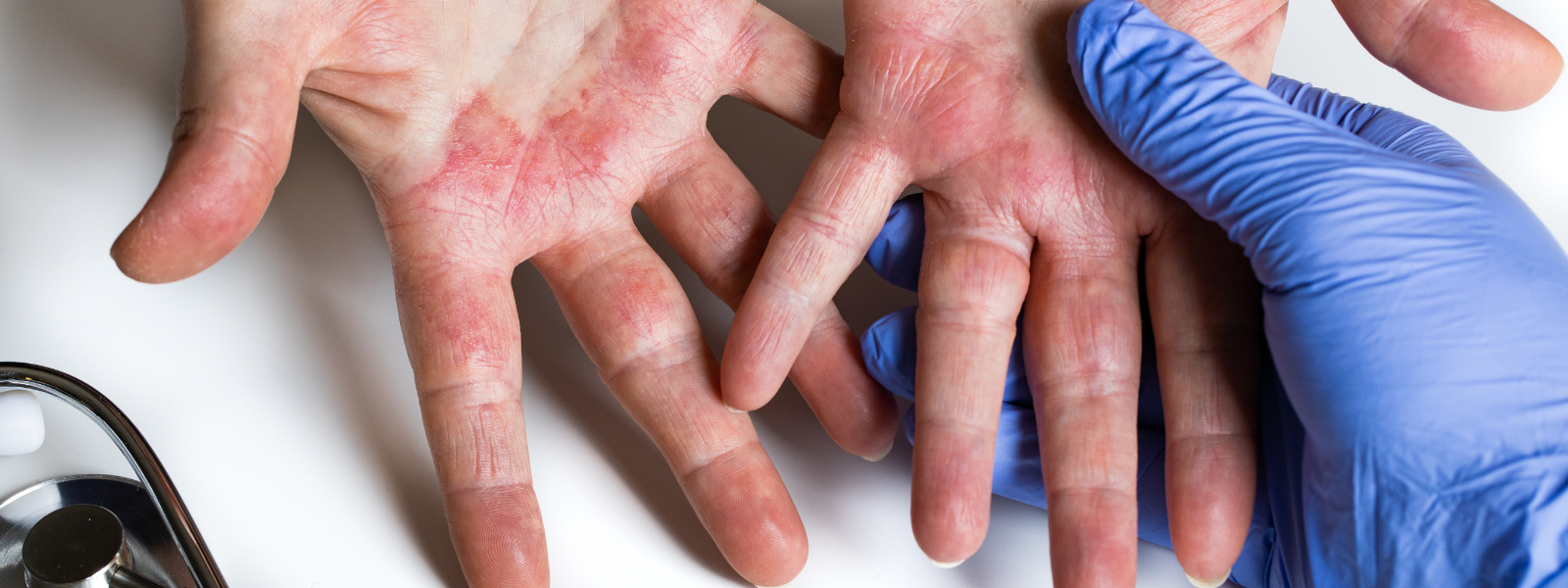
Overview
Eczema Overview
Atopic dermatitis, more commonly known as eczema, is a condition that causes red and itchy skin, but it is not contagious. It is a chronic condition, which means you can experience flare-ups off and on for years, or even a lifetime. You may be at a higher risk of developing atopic dermatitis if you have asthma, hay fever or other allergies. It is also more likely to affect those with a family history of atopic dermatitis. Environmental factors, such as insect bites, harsh chemicals or stress, may trigger an onset.
Eczema is prevalent, with more than 3 million new cases diagnosed each year in the U.S. Its cause is unknown, but researchers believe that atopic dermatitis may be attributed to an overactive response by the immune system. Research shows that some people with atopic dermatitis have a gene mutation that can contribute to this condition.
While anyone can get atopic dermatitis, doctors most commonly diagnose eczema in children. Although there is no cure, treatments are available to relieve itching and avoid new outbreaks.
Symptoms
Eczema Symptoms
Symptoms of atopic dermatitis may be similar to other skin conditions. Some signs may include:
Some people may mistake these as an indication of an allergy.
These symptoms can cause bacterial or fungal infections, loss of sleep, depression or anxiety. It is essential to see your doctor, get a diagnosis and begin treatment as soon as possible.
Diagnosis
Eczema Diagnosis
The first step to diagnosing atopic dermatitis is scheduling a visit with your doctor. Your doctor will examine your skin and ask you about your and your family’s medical history. They will want to know what kind of soaps, detergents, perfumes and cosmetics you use, any medications and supplements you take, if you have problems sleeping and if specific foods seem to trigger any symptoms.
Although not needed to diagnose eczema, your doctor may order blood or other lab tests to rule out other conditions. These tests can help your doctor identify other conditions that could be causing your symptoms or other conditions that go hand-in-hand with your eczema.
Treatments
Eczema Treatments
There are a variety of treatments for eczema, including medications, therapies and lifestyle changes such as:
Medications
- Corticosteroid creams or ointments
- Calcineurin inhibitor creams
- Antibiotic cream for bacterial infections, open sores or cracks
- Oral antibiotics to treat infections
- Oral corticosteroids to control the inflammation
- Injectable biologics to treat people with a severe disease if they do not respond well to other treatments
Therapies
- Wet dressings in combination with a topical corticosteroid
- Light therapy using natural sunlight, artificial ultraviolet A (UVA) and narrowband ultraviolet B (UVB)
Lifestyle Changes
- Moisturizer applied at least twice a day
- Oral allergy or anti-itch medicines such as antihistamines like Zyrtec®, Allegra® or Benadryl®
- Wear gloves and apply bandages to the places where you want to scratch
- Limit your baths and showers to no longer than 15 minutes
- Use warm water when bathing instead of hot water
- Apply moisturizer to damp skin
- Dry off gently by patting your skin instead of rubbing
- Use a humidifier to help keep your skin moist
- Wear loose, cool clothing and avoid rough, scratchy or tight clothing
- Reduce your stress and anxiety through various relaxation techniques or therapy
- Identify and avoid any triggers that cause flare-ups or worsen your condition
- Your doctor may recommend you take a “bleach bath” (be sure to follow your doctor’s directions exactly)
Specialists

